NTDS Mission
To enhance the quality of life for people with kidney failure by engaging nephrologists as team leaders in transformational change that continuously improves the safety of life sustaining dialysis.
 NTDS Projects
NTDS Projects
 Nephrologists as Leaders
Nephrologists as Leaders
 NTDS Spotlight
NTDS Spotlight
New Online Module: Optimizing Hemodialysis Vascular Access Planning
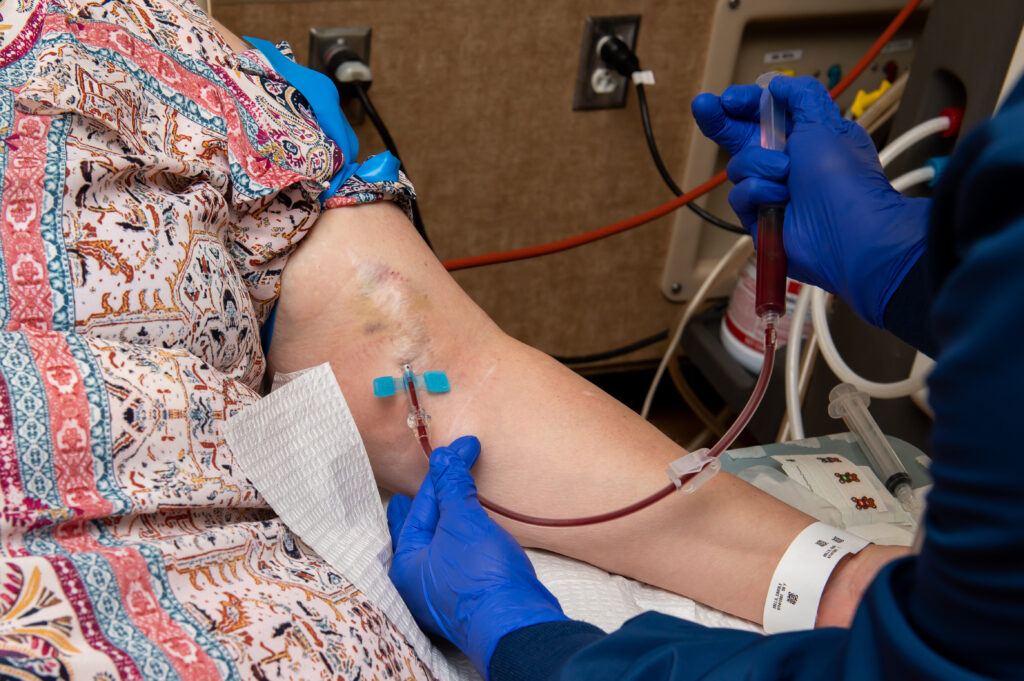
This self-paced learning tool is designed for nephrologists and other staff in an outpatient hemodialysis facility. The module is case-based and focused on a patient-centered approach to improve safety and mitigate infections by reducing catheters.
New Antibiotic Prescribing Online Learning Module
Optimizing antibiotic use can decrease adverse events, improve infection cure rates, and patient outcomes. This case-based resource covers strategies to improve antibiotic prescribing in outpatient dialysis settings.
CE credits are available for those who register and complete the module activity.
Preventing Outpatient Dialysis Infections As A Team: Targeting Zero Infections Micro-Webinar #1

In part one of this three-part micro-webinar series for nephrology fellows, Drs. Sana Waheed and Solomia Savedchuk proffer their insight into team dynamics in the effort to prevent dialysis infections.
COVID-19: Lessons from the Kidney Community

This module describes the experiences of numerous ASN members and volunteers as they navigate the COVID-19 pandemic in the kidney community. The information presented in this module is intended to better prepare the kidney community for future pandemics or other wide-reaching healthcare emergencies and disasters.
 Online Learning Modules
Online Learning Modules
ASN has developed these online learning modules in partnership with the Centers for Disease Control and Prevention (CDC). These self-paced online resources focus on key infection prevention techniques and patient safety concepts in a case-based format.
Antibiotic Prescribing in the Outpatient Dialysis Setting
COVID-19 Lessons from the Kidney Community
 NTDS Resource Library Highlights
NTDS Resource Library Highlights
Updated Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings

Updates have been made to the original HICPAC recommendations from 2014, including:
These core practices are intended to serve as a standard reference and reduce the need to repeatedly evaluate practices that are considered basic and accepted as standards of medical care.
Days Since the Last Bloodstream Infection Poster

Preventing infections is essential for patient safety. Facilities are encouraged to place this poster, tracking the days that have passed since the last bloodstream infection (BSI), in areas visible to patients, family members, and staff to raise awareness about infections. The poster can also be used to start discussions and provide education about the importance of preventing BSIs with patients and family members.

